
Common Bone and Muscle Problems in the Elderly: What Can We Do?
It is inevitable that our bodies deteriorate with age. As we get older, our risk to long-term ailments increases and terms like osteoporosis and osteoarthritis become prevalent in conversations. As much as we try to prevent them, it takes significant lifestyle changes to fully avoid such predicament. This article talks about a few of the most common complaints in the elderly and the options we have for treatment.
Osteoporosis
One of the most common problems amongst the elderly, osteoporosis is a disease where bones become weak and brittle. The bone is a tissue that goes through a breakdown and replacement cycle, and osteoporosis happens when new bone does not form fast enough to keep up with the lost bone, decreasing strength of the bone. This condition increases a person’s risk to fractures caused by falls or mild stresses such as coughing or bending over. The hip, wrist and spine are common areas where osteoporosis-related fractures may occur.
Someone with osteoporosis may experience back pain and a loss of height over time. Women are more predisposed as the reduction of estrogen during menopause is one of the strongest risk factors for developing osteoporosis. However, this condition may also occur in both women or men who have a family history. Those who have eating disorders, have undergone a gastrointestinal surgery for removal of the stomach or part of the intestine and those with calcium deficits are also at high risk of contracting osteoporosis.
Osteoarthritis
This occurs when the cartilage that helps cushion our bones from our Joints wear out. The cartilage prevents bones from rubbing against each other, so when it wears off, the friction causes pain and inflammation. This disease usually affects joints in hands, knees, hips and spine. Even though damage is irreversible. symptoms can be managed. Symptoms can range from pain, stiffness. tenderness. loss of flexibility, bone spurs and swelling.
The elderly are very susceptible to osteoarthritis due to wear and tear of the body. Obese people are at higher risk as heavier individuals have more stress on their weight-bearing joints. Those who have previously suffered joint injuries are also more exposed to osteoarthritis.
Chronic Pain
Persistent or recurring pain is a common ailment amongst the elderly. Pain is a result of osteoarthritis and osteoporosis, but can also be a symptom of many other diseases and occur in other areas such as the head, throat, ears. nerves or wounds. Pain can be debilitating and depressing for the elderly, causing them to retreat from social activities and inhabit them from carrying out simple tasks.
When pain lasts too long, a ‘pain memory’ may develop. The body remembers this pain, enabling stimuli to trigger this ‘memory’ easily. Long-term pain markers also lead to increased sensitivity of nerve cells. This constructs a vicious cycle, spiralling the individual down in pain.
What Can I Do?
When we are faced with pain, many of us instinctively turn to painkillers. Medications such as acetaminophen and anti-inflammatory drugs like NSAIDs can help relieve osteoarthritis. The most common type of drugs used for osteoporosis are bisphosphonates, which prevents the loss of bone mass. Bisphosphonates can be taken orally or injected. Antidepressants are popularly used for chronic pain. Serotonin and norepinephrine reuptake inhibitors (SNRIs) that may be prescribed to relieve chronic pain include duloxetine (Cymbalta), venlafaxine (Effexor XR, Pristiq) and milnacipran (Fetzima, Savella). Anti-seizure medications, such as gabapentin (Gralise, Neurontin, Horizant) and pregabalin (Lyrica) quiet pain signals from your nerve cells, and are helpful for stabbing or shooting pain resulting from nerve damage. For cases of extreme pain, opioids may be prescribed in low doses. Due to the high risk of addiction and overdose, opioids are usually used as a last resort.
Apart from oral medication, other procedures are available for treatment of osteoarthritis. Some people turn to cortisone or hyaluronic injections, that serve to relieve pain and provide some cushioning.
Is going under the knife the last resort?
There are many who have tried the above mentioned options to find relief. If prescribed by a doctor, the definitive treatment would be surgery. Although there are attendant risks, surgery would be the clear cut treatment to align bones or replace joints as that address the problem at its source.
In some cases where the patient cannot or prefers not to go under the knife, MBST therapy would be an option. This is a non-invasive and painless treatment similar to how MRI (magnetic resonance imaging) works. MBST therapy involves the molecular biophysical stimulation of cells and cell groups of a specific type of tissue to foster the affected body cells to auto-rejuvenate and heal.
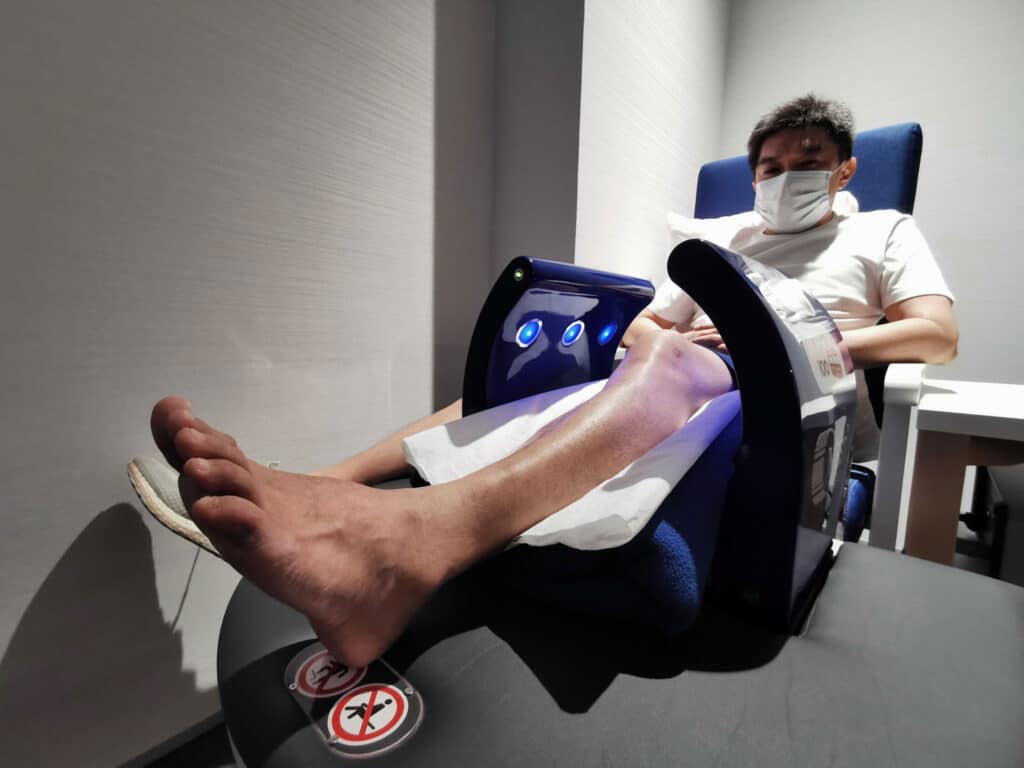

How does MBST help?
As a general principle, MBST therapy transfers energy to the specific aliment region of the body to increase the metabolism and thereby triggers the body’s own repair mechanisms and regeneration processes. MBST therapy hence tackles degeneration, which is one main underlying cause of these musculoskeletal ailments.
The physical principle of MRI is using hydrogen nuclei of cells in our body to take up energy and then energy is released partly into the surrounding tissues. This same principle is applied in MBST to stimulate various biophysical processes and trigger anti-inflammatory and pain-relieving effects.
Where can I get MBST therapy?
MBST therapy is achieved with special devices such as magnetic resonance (MBST) and diamagnetic resonance (CTU), which are available at RejúveMagnetic Specialist Clinic. This medical centre is fully licensed and led by a medical specialist in Anesthesiology who is also a Consultant in Pain Medicine. He teams up with a trained therapist to diagnose and treat your condition. The clinic is also fully-equipped with treatment rooms and facilities to ensure patients have a comfortable and fuss-free experience. Visit rejuvemagnetic.com for more information.
Click here to register your interest and receive a $150 voucher now! (T&Cs apply).






